AIA OVHC
What is AIA OVHC?
Overseas Visitors Health Care Cover (OVHC) is a form of health insurance that is designed specifically for international visitors to Australia. It can be purchased by people who are visiting or temporarily residing in Australia.
AIA offers OVHC to eleven visa subclasses:
- 188 - Business Innovation and Investment
- 400 - Temporary Work (Short Stay Specialist)
- 403 - Temporary Work (International Relations)
- 407 - Training
- 408 - Temporary Activity
- 417 - Working Holiday
- 462 - Work and Holiday
- 476 - Skilled Recognised Graduate
- 482 - Temporary Skill Shortage
- 485 - Temporary Graduate
- 489 - Skilled Regional
Rate Rise: 1st October 2025
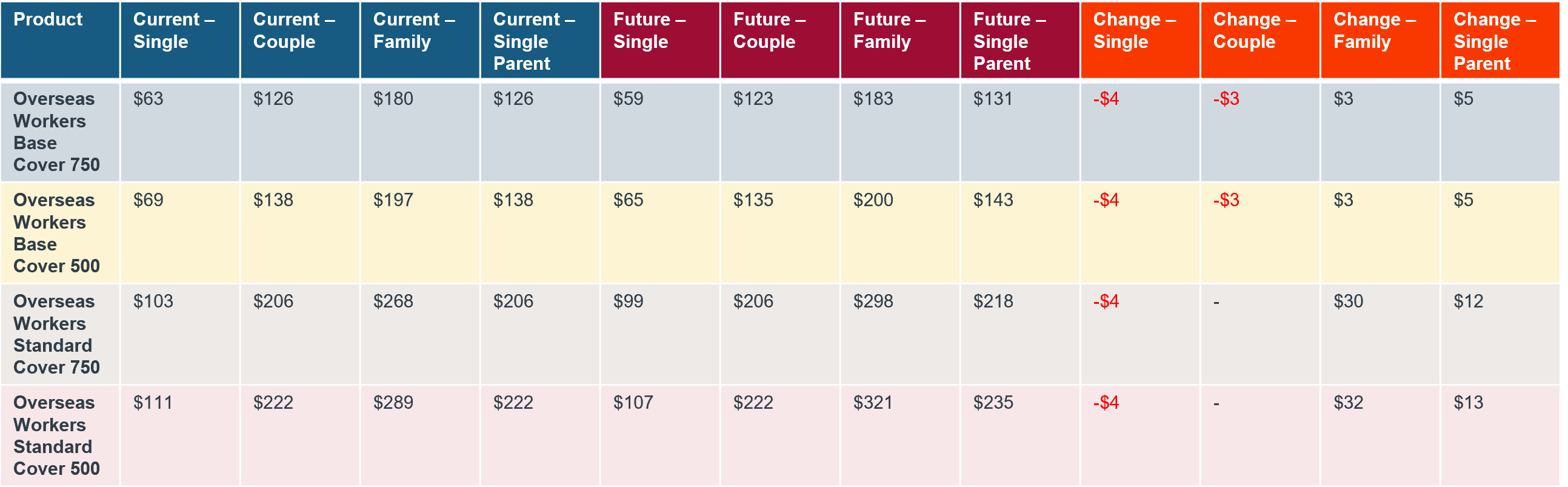
Frequently asked questions
What Outpatient Services are covered?
Allied Health Services Available (per person per Calendar Year)
Waiting Periods & Portability
- For members that don’t have a pre-existing condition there is no waiting period.
- Members must complete the pre-existing conditions determination form(s), prior to surgery. Both GP and specialist forms are necessary consistent with resident cover rules.
- Members who attend an emergency department for urgent care should be aware the Pre-existing Condition check must be completed before AIA Health can confirm benefits are payable.
- We issue transfer certificates to Australian private health insurers and honour waiting periods served.
- A 12 month PEC waiting period will apply for members transferring from an overseas private health insurer.
Transferring Members
What is not covered with AIA OVHC?
- Medical checks, vaccinations, x-rays or pathology for Visa applications
- Outpatient pregnancy services (e.g. ultrasounds, obstetrician consultations)
- Any assisted reproductive services (e.g. IVF, GIFT)
- High cost medicines such as certain Chemotherapy drugs for Cancer treatment are not covered
- Organ transplants
- Cosmetic surgery
- Bone marrow transfusion
- Outpatient psychiatric services
- Services not listed on the Medicare Benefit Schedule
- Non-Allied Health extras – e.g. Dental
RESTRICTIONS: Pregnancy and Birth & Hospital Psychiatric Services
RESTRICTION DEFINITION: If you receive treatment as a private patient in a public hospital OR a private patient in a private hospital, AIA only pay a set amount towards the treatment. You may have significant out-of-pocket expenses for these treatments.
Ambulance Cover
AIA OVHC will pay benefits towards ambulance transportation when medically necessary for admission to hospital, emergency treatment onsite, or inter-hospital transfer for emergency treatment.
It does not extend to transfers due to patient preferences.
AIA OVHC will also pay benefits towards ambulance services in circumstances when immediate hospital or onsite treatment is required for a serious and acute injury or condition where the viability or function of an organ or body part is threatened
Can OVHC access state ambulance cover if wanting comprehensive cover?
AIA Health do not offer standalone ambulance cover.
If an OVHC member wants additional ambulance cover they will need to engage other health funds to understand their eligibility rules.
Payment & Application Options
Policy start dates can be pushed back for up to 7 months to Commencement date must be within 7 months of todays date
Members
can utilize the 30 day cooling off period to terminate cover. AIA Health reserve the right to
retain first month premium as an
administration fee.
Payments are made monthly
or annually only through direct debit via CC.
OVHC
start date:
- Offshore: The date of arrival in Australia is the start date
- Onshore: The date visa was granted is the start date
Dependants
Adult dependents may remain on a family
cover until their 24th birthday
and must take out independent equivalent or lower cover within 60 days to avoid waiting periods.
Newborn Children
A newborn, adopted or fostered child can be added to a
membership without waiting periods provided the main
Policyholder has held the policy for more than two months and
the baby, adopted or foster child is added within six months
of birth/adoption/fostering.
Other child dependants added to a policy will be subject to new waiting periods. This includes children added more than six months after birth, adoption, fostering or marriage. Normal portability rules will apply in the case where a child is transferring from another Australian health fund or registered international insurer recognised by us.
CPAP Type Devices
- You have served the 12-month waiting period
- You have undergone an overnight investigation for sleep apnoea (a sleep study) for which a Medicare benefit would normally be payable for Australian residents
- The device is purchased or hired within the 12 months following the sleep study.
- The device is purchased in Australia.
If the CPAP-type device costs more than the benefit we pay, you will be responsible for paying the remaining amount. A benefit of $500 per member is payable within a rolling 5-year period.
If someone required a Hospital Policy to avoid MLS and is on a Yellow Medicare Card, can we sell both an OVHC and a PHI?
No. HAMBS only allows one membership per person and so the same person couldn’t hold both an OVHC membership and a membership for a Retail Hospital product.
What is Repatriation?
Cover
for repatriation to visa holder's country of origin if they suffer a
substantial life altering illness/injury or become terminally ill after taking
out an eligible product. Limits apply.
Benefits are only payable once approved by
AIA and where the illness or injury was not present in the six months prior to
eligible policy start date.
- Repatriation when alive: Base Cover up to $50,000 and Standard Cover up to $100,000
- Mortal remains or Funeral: up to $10,000.
AIA provides repatriation benefits on both OVHC covers
2 month waiting period for repatriation or funeral expenses, however this will extend to 12 months if relating to a pre-existing condition.
Suspension Rules
Members must be financial with AIA OVHC for a minimum of 3 continuous months in
order to suspend their cover.
Overseas travel
Minimum 4 weeks and maximum 12
months
Financial
Hardship
3 months maximum
Contacts
Customer Service: 1800 161 170 or 03 8803 9961
OVHC Extensions: Sales - 1453, CSC - 1455, Broker - 1458
NHS 24/7 Helpline: 1800 566 091
Customer Service Mailbox: au.myown.claims.support@aia.com
OVHC Email: ovhs.memberservices@aia.com.au
OVHC Claims: ovhs.claims@aia.com.au
